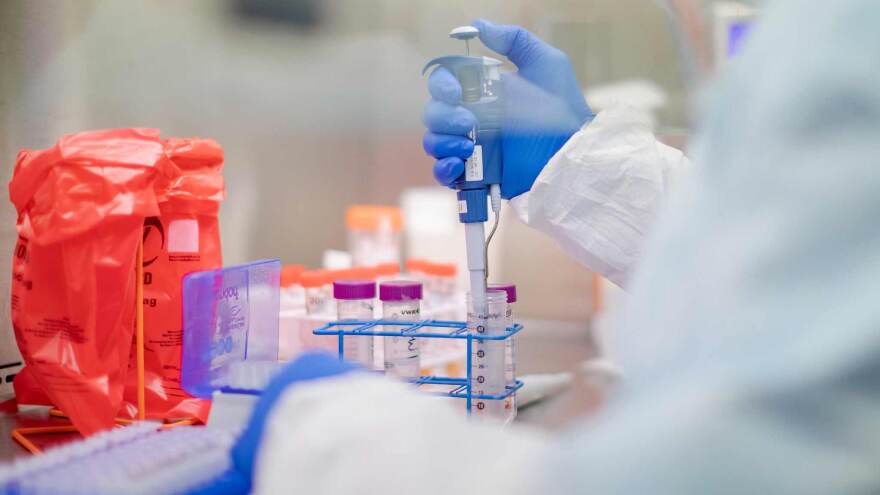
If you’re confused or frustrated by coronavirus testing, you’re not alone.
Following pandemic precautions can seem like chasing a moving target as the public grapples with evolving CDC guidelines, conflicting advice from various experts, government and media, and another spike in online misinformation accompanying the omicron variant surge.
Experts say regular testing is key to curbing the virus’ rapid spread but when COVID surges, the nation's testing capacity struggles to keep up with demand. Many people are unable to find or afford home-testing kits and experience long lines and turnaround delays at PCR testing sites.
The current surge is largely attributed to the swift spread of the virus’ most transmissible variant yet. The U.S. is averaging more than 500,000 new COVID cases a day – much more than any other time during the pandemic.
San Antonio’s 7-day rolling average of new cases has surged 416.5% over the last two weeks. As of Jan. 2, the local positivity rate was 27.3%.
While omicron seems to cause less severe illness among the vaccinated, U.S. hospitalizations have increased more than 50% over the last two weeks. According to San Antonio’s health department, 30% of people hospitalized with omicron are fully vaccinated compared to 20% for the delta variant.
What do you need to know about the various ways to test for COVID-19, how to do so in a timely and accurate way, and common testing pitfalls to avoid?
How soon after exposure should you get tested? What’s the average turnaround time for PCR results in San Antonio? If positive, how long should you isolate?
How long does someone who had COVID continue to test positive afterward, on average? What’s the likelihood of a false negative or false positive?
How effective are rapid tests for detecting omicron? How often should you test? How will insurance coverage for rapid tests work? Why are they so hard to find? What efforts are being made to increase testing capacity?
What should you know about fake test sites, buying rapid tests online and other known scams?
These answers have been edited for length and clarity.
If I’m not feeling well and I get tested, do I need to wait for my results to go back to work?
New testing sites have been opened up to improve accessibility so people can get tested more readily so they're not losing too much time from the workplace. But frankly, if there's somebody that's having symptoms right now — given our local test positivity rate — it is very important that employers support testing to make sure that they're not having ongoing transmission in the workplace.
What is the probability that a rapid antigen test will return a false negative if my rapid antigen test comes out negative? Am I good to go?
It's a complicated answer. Antigen tests are really accurate at telling you if you have an active infection going on. PCR tests are sensitive enough to detect if you have an infection before you're even symptomatic. The PCR test can also detect when you have dead virus. So after you're overcoming your infection, you could potentially test positive for weeks later on a PCR test.
If you've had an infection and you're looking to see if you've cleared that infection so you can return to work, take an antigen test.
If I need to show an airline a negative COVID test for travel, is an antigen test enough?
The scarcity of testing is making things really difficult. So for a lot of travel, air travel in particular, the airlines are requiring testing beforehand. One of the challenges with everybody getting tested is that it's hard to get that turnaround time where you get the results back. Most airlines require the test within 72 hours so that you have a sense that someone is not carrying, not contagious while they're on the plane. If you get further out, they may contract the virus afterwards.
A PCR is the most common version of the molecular test. It's the most sensitive test, but it can take a little bit more time. The rapid tests are usually antigen tests that check a protein in the virus. Now, those turnaround times are faster, but the sensitivity is a little bit less, particularly in asymptomatic people. So what I would recommend doing is checking with your airline to see if they accept antigen tests, because if they do, they definitely give you a faster time.
Do I need to test if I am able to quarantine myself before an event, travel, etc.?
It really depends on what your situation is. The safest thing to do is if you can quarantine at home for 10 days, then you're going to be really outside the infection window. If you develop symptoms at any point, you could get tested. Most people look at testing because they don't want to stay home or quarantine for that time period.
Is the omicron variant really more mild than delta or other previous variants?
So this is not a cold. Omicron is somewhat milder in relation to delta, which we know could cause very severe disease. That being said, we are still seeing people admitted to the hospital. Hospital numbers continue to go up, which is consistent with moderate to severe disease by definition. And we're still seeing people end up in the ICU and on ventilators. People should still take measures to protect themselves and their family members because this is more than just a cold. People can get very ill.
What does “mild” really mean when we’re talking about COVID-19?
You're probably going to get a different answer depending on who you ask. For a lot of clinical studies, they have to have a set definition. Usually if you're requiring oxygen supplementation, additional oxygen just to maintain your oxygen levels, you have by default moved to moderate or severe disease. Mild symptoms are usually described as people who are staying at home, they don't feel great, but they're otherwise OK. They may be minimally symptomatic. But once people start getting sicker to where they're being admitted to the hospital, that's definitely in the severe category.
Then there's a gray zone in between, which is probably where the ambiguity with a moderate definition comes from. Modern definition would be people that are still having symptoms that go beyond five days, so they may have to stay home for a longer time period.
Am I safe standing in line to get tested?
Often lines tend to be outside, so there’s better ventilation, but a mask — especially an N95 — is your greatest tool in protecting yourself.
Spacing is also key. Certainly anybody that's going to any testing center should be wearing a mask. They're in the testing center because they're going to be around other people. Knowing when to get tested is also key. So if you're having symptoms right now, there's a high likelihood it could be COVID. And so it makes sense to get tested if you don't have acute symptoms and you're just wanting to get tested.
What kind of mask should I be wearing now?
The most important thing is that a mask only works when it's worn appropriately, covering the nose and mouth. They don't work as chin straps.
Cloth masks probably provide the least amount of protection, but it's better than no mask at all. Surgical masks or barrier masks that are largely used in health care facilities are good. And then there's the N95 or KN95, and they definitely provide the most filtration and the most protection. It's just important that people wear them consistently. I think that's the biggest challenge is continued consistency with wearing the masks.
Click here for the City of San Antonio’s list of testing sites.
Guests:
- Rudy Arispe, spokesperson for the San Antonio Metropolitan Health District
- Sal Webber, president of Community Labs
- Jason Bowling, MD, associate professor and infectious disease specialist in the Long School of Medicine at UT Health San Antonio and chief epidemiologist at University Health
"The Source" is a live call-in program airing Mondays through Thursdays from 12-1 p.m. Leave a message before the program at (210) 615-8982. During the live show, call 833-877-8255, email thesource@tpr.org or tweet @TPRSource.
*This interview was recorded on Wednesday, January 12.